Eczema Explained: Causes and Classifications
Introduction to EczemaEczema is a term derived from the Greek word ε′κζεμα meaning ‘to boil’. Eczema or dermatitis is defined as an inflammatory condition that can cause redness, itching, dryness, or scaly skin. It is a chronic condition that can have a significant impact on an individual's quality of life due to its symptoms and potential complications. According to the American Academy of Dermatology, eczema affects over 31 million people in the United States alone, highlighting its prevalence and importance as a health concern.
Eczema can manifest in various forms, ranging from mild to severe, and its symptoms can vary from person to person. Understanding the underlying causes of eczema is crucial in managing the condition effectively. By exploring the genetic and environmental factors that contribute to eczema development, readers will gain insight into why some individuals are more prone to developing this skin condition than others.
Types and Symptoms of Eczema-Atopic Dermatitis
Atopic dermatitis is the most prevalent form of eczema, affecting up to 20% of children and 3% of adults in the United States. It is distinguished by the red, itchy, and inflamed skin which leads to the formation of scaly patches, deep cracks, and flaking. Atopic Dermatitis often develops in early childhood but can continue to impact the adult life of the affected individual.
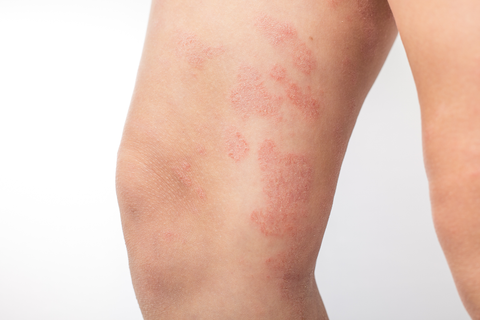
Type of Eczema pictured: Atopic Dermatitis
- Scaly Patches on Skin: Dryness caused by this condition results in scaly patches appearing on the skin.
- Intense Itching: One of the earliest signs is extremely itchy skin which can often result in repeated scratching that at times, the area of skin starts to bleed, thus affecting one's overall quality of life.
- Red or Brownish Gray Patches: Areas of affected skin become red and brownish gray due to intense irritation and inflammation.
- Cracked or Leathery Skin: In more severe cases, skin becomes thickened and leathery and breaks open leading to cracking of skin.
Moreover, it is accompanied by some of the allergic conditions which include hay fever, asthma, and allergic rhinitis (flu, sneezing upon exposure to allergens). Research into atopic dermatitis continues to advance our understanding of this complex skin disorder. Genetic predisposition, immune system dysfunction, environmental factors, skin barrier impairment, and psychosocial factors all play significant roles in the development and exacerbation of atopic dermatitis.
-Contact Dermatitis
Contact dermatitis is an inflammatory skin condition characterized by eczematous reactions, resulting from exposure to chemicals or metal ions with potential toxic effects. This condition can be broadly classified into two main categories: irritant contact dermatitis and allergic contact dermatitis.
Irritant contact dermatitis is a nonspecific reaction caused by direct chemical damage. It can be induced by various factors such as chemical or physical agents and microtrauma. Physical irritants like friction, abrasions, occlusion, and detergents (e.g., sodium lauryl sulfate) can contribute to irritant contact dermatitis.
On the other hand, allergic contact dermatitis is a delayed hypersensitivity reaction to external contact antigens, involving immunological responses. Common allergens associated with allergic contact dermatitis include nickel, balsam of Peru, chromium, neomycin, formaldehyde, thiomersal, fragrance mix, cobalt, and parthenium. In the United States, Poison Ivy is recognized as the most common cause of allergic contact dermatitis.
More than 15,000 substances that come into contact with the skin can trigger allergic reactions, with common culprits being fragrance and nickel found in numerous everyday products.
Both irritant contact dermatitis and allergic contact dermatitis can exhibit three distinctive patterns of presentation:
- Initially: Redness, swelling, oozing, pus, or water-filled bumps.
- Subsequently: Crusting, scaling, and pigmentation.
- Eventually: Skin thickening.
The acute irritant reaction usually reaches its peak quickly, within minutes to a few hours after exposure, and then starts to heal, while in allergic contact dermatitis, the elicitation time depends on the characteristics of the sensitizer, the intensity of exposure, and the degree of sensitivity. Lesions usually appear 24 to 72 hours after exposure to the causative agent and reach their peak at approximately 72 to 96 hours. Allergic contact dermatitis improves more slowly than irritant contact dermatitis and then recurs faster (in a few days) when exposure is re-established.
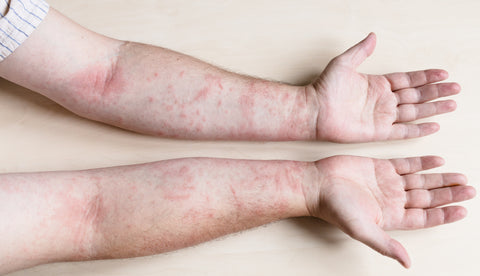
Type of Eczema pictured: Contact Dermatitis
Symptoms
Symptoms of contact dermatitis usually occur within hours after coming into contact with the triggering agent. They may include:
- Redness and raised bumps on the affected areas of the skin
- Intense itchiness and burning skin
- Tender and swollen skin.
The symptoms persist for several days if left untreated. At times, those who regularly come into contact with the triggering agents, are generally at a higher risk of developing chronic contact dermatitis, which must be taken care of and managed effectively as it may continue for a long time.
Understanding the causes and triggers of contact dermatitis is essential for effective management and prevention of flare-ups. By educating individuals on how to identify and avoid irritants and allergens that can exacerbate their condition, healthcare providers can help patients better manage their symptoms and improve their quality of life.
-Dyshidrotic Eczema
This type of eczema is distinguished by small blisters that are formed on the affected areas, especially on the toes, palms, and feet. Women are more likely to have this form of dermatitis compared to men, especially those who have had atopic dermatitis and allergies in the past.
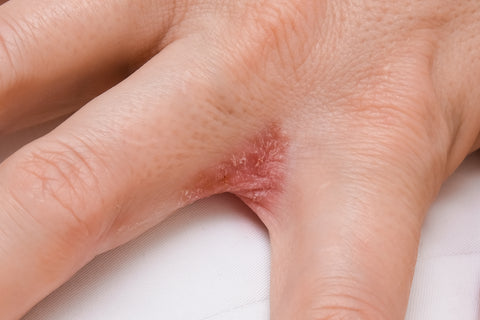
Type of Eczema Pictured: Dyshidrotic Eczema
Symptoms- Small blisters that appear on the soles of the feet, palms, and fingers
- Blisters which usually occur in clusters are often itchy, painful, and filled with interstitial fluid
- Flaky and scaly skin after blisters burst
Various contributing factors can increase the risk of developing this form of eczema such as coming into contact with certain triggering chemical agents, anxiety, stress, and sudden shifts in temperature and humidity levels.
It is important to note that dyshidrotic eczema can coexist with other types of eczema, such as atopic dermatitis or contact dermatitis. By understanding the unique features of dyshidrotic eczema, healthcare providers can work closely with patients to create customized treatment plans that best suit their needs and lifestyles.
-Nummular Eczema
This form of eczema is a distinctive one as it forms circular-shaped patches scattered over areas of the affected skin accompanied by itchiness and burning sensation. It affects men more than women especially those who have had atopic dermatitis and dry skin.
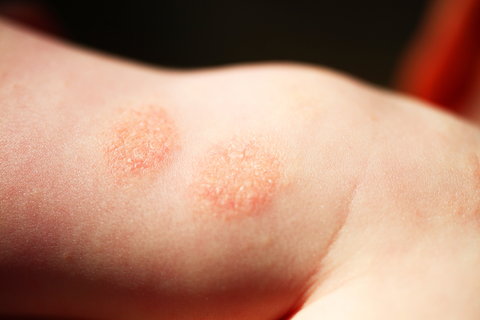
Type of Eczema Pictured: Nummular Eczema
SymptomsThe symptoms of nummular eczema include:
- Round or oval-shaped patches of inflamed skin
- Itching and burning sensation
- Dry, scaly skin
- Crusting or oozing of lesions
It can be triggered due to contact with certain chemicals and irritants including soaps, soap powder, and sudden changes in temperature and humidity levels. By understanding the triggers and symptoms of nummular eczema, individuals can take proactive steps to manage their condition effectively and improve their quality of life.
-Seborrheic DermatitisThis form of eczema primarily occurs on the areas of skin which has a higher proportion of oil glands, the largest being on the face and scalp, as well as the chest. Men are more likely to be affected by it than women specifically those who have had to deal with atopic dermatitis in the past as well as have oily skin.
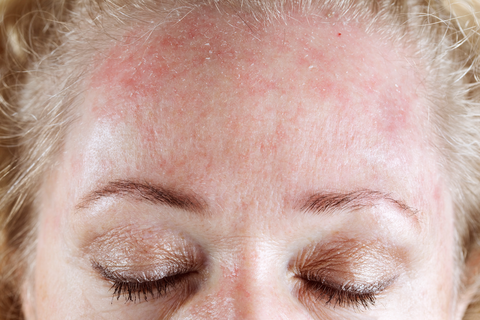
Type of Eczema pictured: Seborrheic Dermatitis
SymptomsThe symptoms of seborrheic dermatitis include:
- Itchiness, redness, and a burning skin
- Crusty Patches of greasy skin
- White flakes scattered across one's scalp
Seborrheic dermatitis is most likely to happen when one is dealing with stress or hormonal imbalance, and its likelihood is also dependent on the changes in weather conditions, or seasons.
Comparison of Different Forms of Eczema
A comparison table for different forms of eczema is given below:
|
Type of Eczema |
Features |
Major Causes |
|
Atopic Dermatitis |
·Most common form of eczema. ·Develops in early childhood but can prevail into adulthood |
·Family history and genetic causes. ·Coming into contact with triggering agents |
|
Contact Dermatitis |
·Rashes and raised bumps on the affected areas of the skin ·Intense itchiness and burning skin |
·Exposure to certain triggering agents such as chemicals, metals, etc |
|
Dyshidrotic Eczema |
·Characterized by small blisters on the hands and feet |
·Stress, exposure to chemicals, changes in temperature or humidity |
|
Nummular Eczema |
·Presents as coin-shaped patches of irritated skin |
·Exposure to irritants, changes in temperature or humidity |
|
Seborrheic Dermatitis |
·Affects areas rich in oil glands such as the scalp, face, and chest |
·Stress, hormonal changes, changes in weather or season |
Each type of eczema has its unique characteristics and triggers that can aggravate symptoms, making it essential for individuals to recognize the specific type they are dealing with. By understanding the differences between the types of eczema, healthcare professionals can develop personalized treatment plans tailored to address the unique needs of each patient.
Causes of EczemaEczema is a complex skin disorder with multiple contributing factors. It's crucial to have a firm grasp and relevant knowledge regarding the difference between each type of eczema to help come up with an appropriate treatment plan suited to each patient's needs. Moving forward, we shall discuss and analyze the main contributing factors that can lead to eczema which include genetics and family history, environmental factors, immune system disorders, emotional factors, and skin barrier dysfunction.
-Genetic and Family HistoryIt has been proven that eczema is relatively more common among those who have at least one parent affected by it. This genetic element raises the possibility of getting eczema threefold, and if both parents have it, then this probability increases tenfold. Specific genes linked to eczema include filaggrin gene mutations, which play a crucial role in maintaining the skin barrier function.
-Skin Barrier DysfunctionA skin barrier serves the purpose of forming a protective layer on the skin preventing external insults. A compromised skin barrier allows moisture loss and facilitates the entry of allergens and irritants, leading to eczema flares. Filaggrin deficiency is a well-known factor causing skin barrier dysfunction in eczema patients.
-Immune System DysfunctionAn Immune System Dysfunction also serves as a contributing factor for causing eczema. Patients affected with eczema have higher levels of pro-inflammatory cytokines, responsible for inflammatory reactions such as IL-4, IL-13, and TNF-Alpha. This is further aggravated by the presence of impaired T cells as they cause the process of inflammation to go on.
-Stress and Emotional FactorsPsychosocial factors, such as stress and anxiety, can negatively impact eczema outcomes. Chronic stress leads to elevated cortisol levels, which suppress the immune system and further exacerbate eczema symptoms. Moreover, psychological distress can result in poor self-esteem and quality of life among eczema sufferers.
-Environmental Factors- Irritants: Soap, shampoo, detergent, and solvents can disrupt the skin barrier and worsen eczema symptoms.
- Allergens: Pollen, animal dander, mold spores, and food allergens can induce eczema flares.
- Temperature and Humidity: Extreme temperatures and low humidity can compromise the skin barrier and provoke eczema outbreaks.
This article provides a comprehensive insight into the significance of eczema, its types, and symptoms. Every type of eczema possesses specific features and has a set of triggering agents that can increase the risk of getting eczema or make the symptoms worse. Therefore, a thorough understanding of the distinct differences between various forms of eczema is crucial to determine which treatment is characterized to be the most suitable to the patient’s needs. Moreover, it is essential to have an educational awareness regarding the different types of eczema to better manage one’s symptoms, which will have a positive impact on one’s quality of life.
These recommendations are not sponsored. They are the result of Dr. Heather D. Rogers, MD evidence-based research and extensive clinical experience.
To learn more, sign-up HERE to receive weekly educational newsletters from our founder and dermatologist, Dr. Heather D. Rogers, MD.
The information on doctorrogers.com and our social media channels, including articles, newsletters, videos, blogs and related links, are provided for general information and educational purposes only. There is no doctor-patient relationship implied and it is not a substitute for obtaining medical advice from your physician. Use of this information and recommended products on this site is at your own risk. Further, their use indicates your agreement with the Terms and Conditions of doctorrogers.com. There is no intent to diagnose or treat any specific medical problem through any of the information shared. Additionally, information shared here is not an extension of the medical care Dr. Rogers provides at her practice.
Citations:
- American Academy of Dermatology Association Eczema Resource Center https://www.aad.org/public/diseases/eczema
- American Academy of Dermatology Association Eczema: Types and treatment https://www.aad.org/public/diseases/eczema/types
- American Academy of Allergy, Asthma & Immunology Contact Dermatitis | Symptoms, Treatment & Management https://www.aaaai.org/conditions-and-treatments/conditions-dictionary/contact-dermatitis
- National Eczema Association Dyshidrotic eczema: symptoms, causes, and treatmenthttps://nationaleczema.org/eczema/types-of-eczema/dyshidrotic-eczema/